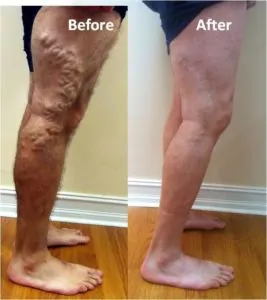
Does insurance cover varicose vein treatment? In a word…yes!
Treatment for varicose veins, venous insufficiency, and venous ulcers is covered by most commercial insurance plans – like United Healthcare, Aetna, Blue Shield of California, Cigna, and Anthem Blue Cross – and government insurance programs like Medicare, but insurance companies like United Healthcare typically want to make sure that you are not seeking varicose vein treatment simply for cosmetic purposes. No insurance covers cosmetic sclerotherapy for spider veins. Insurers want to ensure that you do have real varicose veins and a situation where the circulation is causing you some sort of symptom or problem with your skin or legs. Even if you don’t have visible varicose veins and have totally normal appearing legs, you may still have symptoms of vein disease caused by venous insufficiency. Venous insufficiency is the root cause of varicose veins, a condition where blood flows backwards in the vein (also called reflux) and pools in the lower legs instead of circulating effectively back to the heart.
When will insurance companies cover treatment?
Insurance companies like will typically cover treatment if you have:
- Leg pain
- Leg swelling
- Leg cramping
- Leg heaviness
- * Restless Leg Syndrome
- Skin discoloration around the ankles (venous stasis)
- Leg wounds (venous ulcers)
Symptoms associated with varicose veins and venous insufficiency are usually worse with prolonged standing and at the end of the day. It is very common to hear from patients that pain in the legs or leg cramps interrupt sleep. One of the things that needs to be documented for varicose vein treatment to be covered by insurance is that the patient’s symptoms need to be clearly documented including whether they have pain and, if so, where that pain is. The pain is often described not as a focal pain but as discomfort like heaviness or aching. This can sometimes be severe.
Each insurance company has specific requirements (and they are all different!) for covering varicose vein treatment including some ultrasound requirements like the size of the veins and how much backwards flow, or reflux, there is. As part of your initial evaluation, Dr. Malvehy will perform a detailed ultrasound examination to identify and document the source of your varicose veins and venous insufficiency. This is then provided in documentation to your insurance company to support pre-authorization for treatment.
We regularly work with insurance companies to get pre-approval for patients seeking varicose vein treatment so we understand the different requirements that each insurance company has.
For patients seeking varicose vein treatment with insurance, we work directly with:
- United Healthcare
- Cigna insurance plans
- Aetna insurance
- Blue Shield of California
- Anthem Blue Cross
- Healthnet Insurance Plans
- Tricare for military personnel and their families
- Many others
In addition to these private commercial insurance plans which cover varicose vein treatment, we also work with:
Unfortunately, we are not part of the Kaiser Permanente of physicians and, though you can get varicose vein treatment with Kaiser Permanente, we are happy to offer our services to Kaiser patients with a reduced fee.
Our office accepts most major commercial insurance, Medicare, and MediCal, allowing patients with these insurance plans to see Dr. Malvehy, consistently rated one of the best vein doctors in California. Though our office does not offer vein treatment as part of the Kaiser Permanente network, we offer preferred pricing for patients covered by Kaiser.
The process for getting varicose vein treatment covered by your insurance, Medicare may seem like a long and frustrating one with insurance companies issuing denials for claims or pre-authorizations for the procedures. Often, this happens because the physician or the physician’s office is not familiar with the requirements that different insurance companies have for covering varicose veins. Almost every major commercial insurance company – companies like Aetna and Anthem Blue Cross – covers treatment for varicose veins, including venous insufficiency and venous ulcers, but they all have different guidelines for treatment and want to see different things documented in the patient’s chart before they will agree to cover treatment.
Our office routinely deals with insurance company, Medicare to ensure that our patients can get the vein treatment they need covered by their insurance, including:
- Laser varicose vein treatment
- Minimally invasive varicose vein removal
- Foam sclero-ablation for varicose veins, venous ulcers, and venous insufficiency
Because we have experience getting approval for varicose vein treatment by insurance, our office can make the process as painless for you as possible.
If you need varicose vein treatment covered by Medicare, our staff will ensure that you meet all the necessary treatment guidelines for varicose veins and venous insufficiency as issued by Medicare before initiating treatment. Typically, patients have to have undergone a period of conservative (non-intervention) management of their varicose veins like using compression stockings, trying leg elevation, and attempting to reduce weight. It is also important that patients have documented symptoms or injuries like venous ulcers as a function of their varicose veins – it cannot just be a cosmetic treatment.
Commercial insurance companies like Cigna, Anthem Blue Cross, and Blue Shield of California also cover varicose veins but their requirements are typically different from Medicare. In addition to requiring that physician offices contact the insurer and obtain pre-authorization approval for varicose vein treatment, commercial insurers may also want specific things to be documented including:
- For United Healthcare, varicose veins have to be measured in a certain part of the leg on ultrasound in order to qualify for coverage
- For Blue Shield of California to cover varicose vein treatment, certain language pertaining to the origin of the varicose veins must be included in the ultrasound documentation.
Vein Treatment Evaluation: What to ask?
Considering the sheer number of insurers that may cover varicose vein treatment, it is important that your physician understand the right things to ask you when performing your varicose vein evaluation and documents your visit accordingly. If treatments are performed and not authorized properly, insurance companies may deny coverage resulting in surprise medical bills which can be thousands of dollars, so it pays to go to a specialist location which is expert in vein treatment.
Because Medicare does not require a pre-authorization for procedures, your treatment can usually begin promptly after you have completed a period of conservative management. Obtaining prior authorization for varicose vein treatment from commercial insurance providers like Anthem Blue Cross, Aetna, Cigna, or United Healthcare typically requires about between one and three weeks, so your procedure will be scheduled for a couple of weeks after your consultation and completion of conservative management.
No insurance company covers treatment for spider veins, hand veins, or facial veins. Vein treatments covered by insurance are performed in the office, take an hour or less, and do not have any downtime. If you come to our office, Dr. Malvehy will be in touch with your primary care provider so they are aware of your treatment plan and can coordinate any ancillary care as necessary.
Though varicose vein treatment is covered by insurance companies like Anthem Blue Cross, Blue Shield of California, Cigna, and United Healthcare, they often require their members (patients) to pay co-insurance, co-pays, or deductibles as part of their care. Our office is absolutely dedicated to making sure you understand what you will be responsible for BEFORE you go through with treatment – no one likes a surprise bill in the mail. When you call to make an appointment, our staff will take your insurance information and contact your insurance plan directly in order to give you a breakdown of what we estimate your visit will cost. We can only provide an estimate because insurance plans are highly variable and subject to change but we will do our absolute best to be transparent in the billing process.
Co-pays
Co-pays are payments required by insurance companies every time you visit the doctors office. For a specialist like Dr. Malvehy, these payments usually range $25-75. Some insurance plans have no co-pays while others are as high as $100.
Deductibles
Deductibles are a dollar amount that insurance companies require patients pay out of pocket before their insurance will kick in. Many insurance companies enroll patients in “high deductible insurance plans” where their members will be required to pay several thousand dollars before insurance will kick in. If you have a deductible, this out of pocket expense must be met before your insurance will begin to pay for your visits. Deductibles reset every year and your healthcare spending during the year goes towards that deductible. For example, if you have a $3,000 deductible and you and your family have spent $2,750 on doctor’s visits and medications already in a year, you would have to pay an additional $250 out of pocket before your insurance would make any payments on your behalf. Deductibles are different for everyone. Some plans have family and individual deductibles while others don’t have any deductible at all. This is part of what we will talk to your insurer about before your first visit so you don’t have any surprise charges after the fact. We want you to make an informed decision.
Co-insurance
Co-insurance is another mechanism for insurance companies to require people to pay out of pocket for their care. If you have 10% co-insurance, you will be responsible for 10% of the estimated charges for your visit. For example, if your visit charges are estimated at $150, you would be responsible for $15 at the time of your visit. Insurance and co-insurance typically kick in after deductibles are met so you are responsible for meeting your deductible first. Co-insurance ranges from 0% to 30%, typically, and all plans our different.
We get it. Having your varicose vein treatment covered by insurance can seem complicated. That’s why we go to so much effort to make the process as painless and transparent for you – our patients – as possible. If you need varicose vein treatment and have Kaiser insurance, don’t have insurance or are looking for other options, our non-insurance rates are the most reasonable in the Bay Area and include follow up care (no surprise charges). Call our office at (925) 494-0898 for information on scheduling your appointment.